Game Changers: EMS Technology for Better Patient Outcomes
Key Takeaways
- A fire department’s implementation of a whole blood program will benefit from the use of a new monitor/defibrillator that allows the creation of a custom dashboard menu that can look at hemoglobin levels and Pleth variability indexes to see how a patient would benefit from a fluid challenge or a blood transfusion.
- Training of EMS personnel who have no experience with point-of-contact ultrasound improves when a device’s operation is simple and its design omits the buttons and knobs that are typical of ultrasound systems that are found in hospital emergency departments.
- When a mechanical tourniquet is used instead of a conventional windlass tourniquet, the time that EMS providers must devote to that treatment is decreased substantially, which allows those individuals more time to attend to other patient needs.
The strain on fire service members that’s a result of a continual surge in medical calls is substantial. Besides the bottom-line relentlessness of the calls, the challenges of patient treatment can, to say the least, be exhausting. There seemingly is no relief in sight for the former, but the brilliance of companies that produce the devices that are in responders’ toolbox provides ways to better prepare those folks who are en route to an emergency and to have them walk away feeling very good about the treatment that they administered.
Capt. Mike Dawson is with the EMS Division of the North Metro Fire Rescue District (NMFRD) in Broomfield, CO. The progression and growth of EMS, he tells Firehouse, drives him and his team members. In sharing that, Dawson speaks for many, including representatives of other departments who were interviewed for this article as well as experts in EMS technology.
Message received
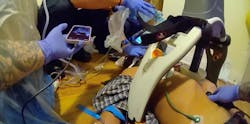
The NMFRD recently began training on the use of ZOLL Medical’s Zenix monitor/defibrillator, which was introduced in September 2025. Among other benefits to the department, the device will aid the agency in the rollout of its whole blood program as early as April 2026.
The device’s capability to allow NMFRD EMS providers to create custom dashboards means that they can look at hemoglobin levels and Pleth variability indexes to see exactly how a patient would benefit from a fluid challenge or a blood transfusion of one unit or more.
“We’re going to be able to use a Pleth variable index probe to determine with confidence that the patient falls within the criteria for whole blood products,” Dawson explains. “That gives our providers more confidence that the treatment is going to work.”
That’s music to the ears for Kristi Hallowell of ZOLL Medical. The development of the Zenix and the company’s Autopulse NXT mechanical CPR device was based on customer feedback that her company embraced with vigor. For example, the Zenix is the successor to the company’s X Series devices. Hallowell tells Firehouse that the company’s developers were so committed to serving users that over-engineering in some ways detracted from seamless application. For example, the way that the carrying bag of X Series models was structured, the device printed into the bag. “That was a pain point for the market,” Hallowell says. The company changed the location of the printer and went back to a previous style of printer paper.
Ease of use also was front and center in engineers’ development of the Autopulse NXT’s design for “resuscitation on the move.” Hallowell says, “If a patient is in a tight space and providers need to take them down a flight of stairs or if the patient is in a high-rise building and must go down in an elevator, which requires the patient to be positioned in such a way that they’re upright or at an angle, the device continues to provide the capability to continue to do high-quality CPR.”
Dr. David Rayburn, who is medical director for the New Orleans Fire Department and New Orleans EMS, can relate based on his experience with Butterfly Network’s iQ3 portable ultrasound device. Familiar with ultrasound in the hospital environment, Rayburn commends the company for its elimination of all of the “knobology” that’s associated with big ultrasound machines that are in emergency departments (EDs).
With the iQ3, EMS providers “can change the gain and the depth without the need for buttons and knobs that, honestly, the prehospital environment doesn’t need,” Rayburn explains. “With iQ3, if you want to make the screen brighter or darker, you can increase the gain just by moving your thumb left and right. If you want to go deeper, you move your thumb down. If you want to go more shallow, you move your thumb up.”
In regard to a FAST (Focused Assessment with Sonography for Trauma) exam, he praises Butterfly Network’s engineers’ incorporation of all of the presets that tell the ultrasound-on-chip technology of the iQ3 how to adjust the depth and gain settings to make sure that the EMS provider is obtaining the best image.
“When you’re training somebody who has no experience on ultrasound, having this simplistic way to do it allows for faster uptake of the information,” Rayburn explains.
Rayburn’s experience with ultrasound in the ED is key to him ramping up New Orleans’ firefighter/paramedics and EMTs on the use of ultrasound on scene and en route to the hospital. Tom Sanger of Butterfly Network finds this to be immensely beneficial in particular to the iQ3 and in regard to point-of-care ultrasound in general.
“The people who are teaching the paramedics to use these tools are the emergency medicine physicians who went on our website and bought their own probe,” Sanger says. “We’re seeing medical directors stand up and say, ‘This is the right thing to do for patients, and we’re not going to wait for the status quo to do it for us,’ on a state by state and agency by agency basis.”
Key to this is Butterfly Networks’ engineers meeting the clinical requirements of the ultrasound machine in the ED that costs tens of thousands of dollars but in a device that costs $3,000–$5,000 that’s mobile friendly.
“It’s game-changing,” Sanger proudly states. “It’s fundamentally unlocking the things that they always wanted to do with mobile ultrasound devices but haven’t had the technology to do.”
Alleviating the chaos
The challenge of limited staffing pervades the fire service and EMS. The latest technology that’s available to firefighter/paramedics and EMTs softens this blow. Take Pafford Emergency Medical Services, which is headquartered in Hope, AR. In the past, the agency relied solely on manual chest compressions on cardiac arrest responses. In many of the rural areas that it serves, volunteer fire departments have limited resources to assist. Around 2020, the agency implemented the use of Defibtech mechanical CPR devices. A couple of years ago, it transitioned to the supplier’s new ARM XR device.
“As a prehospital clinician, we know the No. 1 goal throughout the whole resuscitation process is to minimize pauses in chest compressions,” Gavin Hall of Pafford
EMS says. That can be difficult for two individuals to do as well as manage an airway, administer medications, conduct rhythm analysis and maintain a high awareness of safety. “Without the burden of physical labor, we can focus all of our efforts on other areas … and, ultimately, achieve a return of spontaneous circulation,” Hall notes.
As a result, Pafford EMS teams no longer emerge from calls physically drained.
Hannah Herbst, who is the CEO of Golden Hour Medical, tells Firehouse that freeing up the hands of EMS providers who respond to a call that requires the need to apply a tourniquet was part of the creation of the AutoTQ mechanical tourniquet.
“Windlass tourniquets, although lifesaving, are not only hard to use, they are time consuming,” Herbst says. “The time on task that’s required to tighten the tourniquet, the proficiency to use it effectively, the number of tourniquets that might be needed: There was room for improvement.”
Pressing just one button activates the AutoTQ, which “frees up the hands of the EMS provider to treat other injuries,” Herbst states.
Brenda Lodermeier is a firefighter with the Rockville, MN, Fire Department and a former assistant fire marshal with the St. Cloud, MN, Fire Department. She’s in the process of distributing eight AutoTQs to Minnesota fire departments.
“The unit talks to you, so it’s almost like having a dispatcher in your ear,” Lodermeier explains. Once the device is employed, “The EMS provider can start putting in IVs and check other things and can attend to other injuries.”
She concedes that the cost of the AutoTQ compared with that of a basic tourniquet can prompt reluctance when departments are presented with the option, “But you’re comparing day and night” in terms of effectiveness and efficiency, she states.
Herbst adds that reluctance also can come into play when members test the AutoTQ on manikins and they don’t get a reading on the device.
“Manikins by design aren’t anatomically correct and are built for use with narrow, windlass tourniquets, not wide, pneumatic tourniquets, such as the AutoTQ,” Herbst says.
The wider cuffs of the AutoTQ require much lower pressures to stop bleeding in the range of 190–250 mmHg. The AutoTQ is set slightly above that to account for any under tightening of the cuff or any movement under stress.
“Manikins also often require precise tourniquet placement on one specific spot to be effective,” Herbst adds.
As to cost, Herbst and Lodermeier point to Golden Hour Medical’s replacement of a used arm cuff or leg cuff at no charge.
“Every time that you buy a new cuff for an AED, you’re talking $50 or $100 or $125,” Lodermeier says.
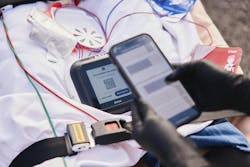
Avive Solutions’ Avive Connect AED was introduced in 2023 for dissemination in public spaces. However, the device’s direct integration with 9-1-1 emergency communications centers via cellular and Wi-Fi connectivity means that EMS providers who respond to an emergency where an Avive Connect AED was deployed are informed en route that the call truly is a cardiac arrest and whether a shock was administered and, if so, how many shocks were administered.
“Typically, field responders show up at a call just based on whatever the caller relayed verbally to the 9-1-1 telecommunicator,” Kat Perry of Avive Solutions explains. “Our device is a pretty awesome way for EMS crews to have that certainty and confirmation that they’re responding to a cardiac arrest.”
Once a crew arrives and the Avive Connect AED is powered off, a QR code shows up on the screen of the device. It can be scanned with a smartphone or tablet, and a full incident report, including when the device was powered on, when the pads were placed on the patient and the full ECG rhythm, is generated.
“The presenting rhythm informs a lot of the care the patient is supposed to respond to,” Perry tells Firehouse.
Consider the boost to responder morale that this provides, she adds.
Reducing assumptions
In circumstances in which time is of the essence, anything that helps firefighter/paramedics and EMTs to zero in more quickly on patient status and needs is invaluable. Those folks and their supervisors should know that opportunities to improve patient outcomes—and to ease the mental burden on responders—are plentiful.
“Anytime that we can simplify things for our providers, we’re going to have more success,” NMFRD’s Dawson states.
“We talk a lot about the cognitive load that providers carry,” Hallowell adds, “particularly when we’re talking about calls that they don’t see often.” She terms the company’s efforts in this regard as decision support and “how clinicians are able to see information right on the Zenix’s screen when they need to.”
Says Sanger about this and iQ3’s role even beyond cardiac arrests: “The agency or the fire department that’s in a rural setting that’s not 100 percent sure on what’s wrong with the patient and whether to move the patient to the local hospital or to a hospital that has more advance clinical services can visually inspect the patient’s anatomy, to see whether there’s abdominal bleeding or other major issues, particularly in the instance of trauma. Otherwise, it’s very difficult to make a very informed decision on such patients. Why listen and guess when you can see and know.”
“I’m a huge proponent of prehospital ultrasound,” New Orleans EMS’ Rayburn says. “Something that’s common that paramedics encounter is shortness of breath. The iQ3 gives EMS providers an opportunity to dramatically alter their treatment pathway without just relying on treating that wheeze and then reassessing. ‘Instead of giving this person a bunch of DuoNebs for pulmonary edema, let’s just given them some nitroglycerin instead.’”
“One of the benefits of AutoTQ is there isn’t as much guesswork and variability,” Golden Hour Medical’s Herbst says. “Studies have found up to an 84 percent failure rate with windlass tourniquets right after training. We have 256 users of AutoTQ that did our training in the past few months, and their average time to apply it from the kit to the wound is 22 seconds.”
“It really makes a difference between life and death,” Lodermeier states, “because somebody stood up and grabbed the bull by the horns to try to save somebody’s life.”
About the Author
Rich Dzierwa
Managing Editor, Firehouse Magazine
Rich Dzierwa joined Firehouse Magazine in 2019 after four tenures with other publications. He was editor-in-chief of Consumers Digest/ConsumersDigest.com and of trade magazine Cutting Tool Engineering. He served as the consumer products reporter for BridgeNews and began his publishing career with an 11-year tenure at Appliance magazine, where he rose to managing editor after serving in other roles. Dzierwa's experience with consumer products, including furnishings, appliances, electronics and space design, has transferred to his Firehouse work regarding the magazine's Station Design columns and the Station Design Awards. Previous work also has contributed to his supervision of several surveys of fire service/EMS members, to produce unique reporting for Firehouse's audience. Dzierwa earned a bachelor's degree in English from Columbia College Chicago.